This promotional material is intended for UK Healthcare Professionals only.
BOTOX® (botulinum toxin type A) Prescribing Information and adverse event reporting information can be found below.
BOTOX®: For treating neurogenic detrusor overactivity (NDO)5
BOTOX®: significant improvements for NDO patients5,6,7
Reduce the impact of NDO symptoms on your patients’ lives.
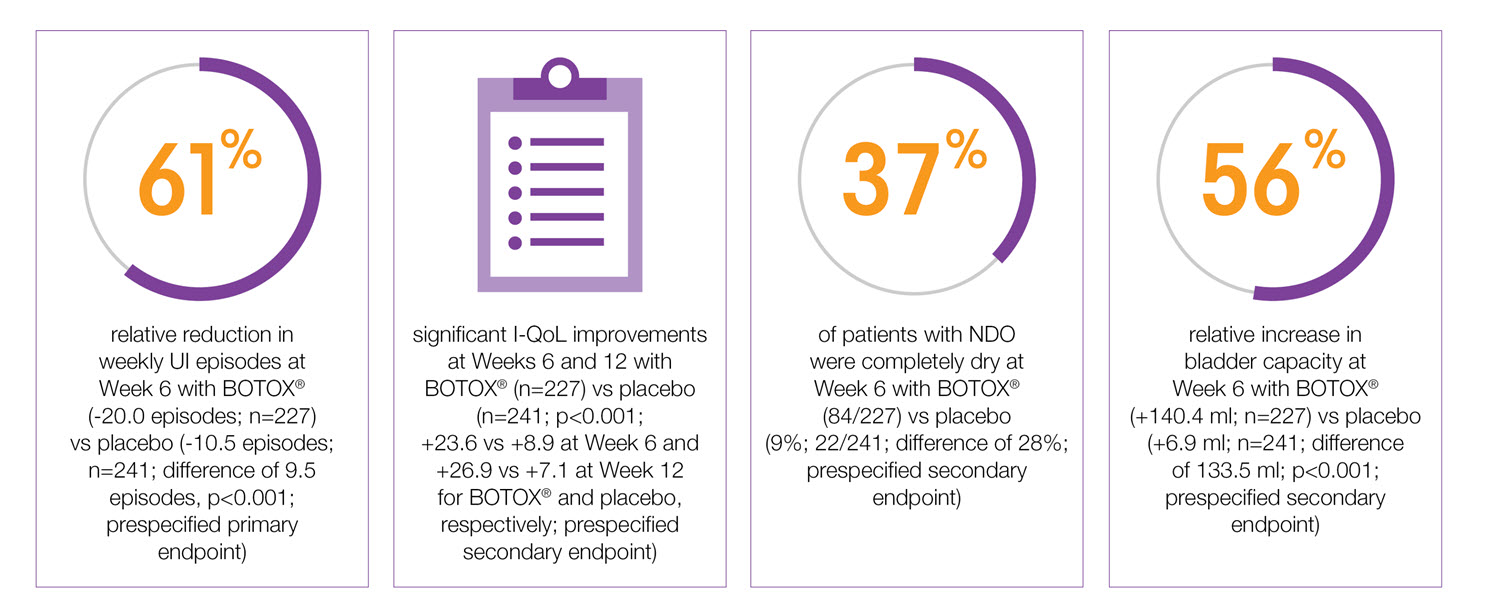
Study context: Pooled analysis of two double-blind, placebo controlled, randomised phase 3 clinical studies, in 691 patients with urinary incontinence due to NDO. To assess the efficacy, safety and effects on quality of life of BOTOX® patients with NDO. Mean baseline weekly frequency of UI: 32.4 BOTOX® and 31.5 Placebo.5
3 reasons to trust BOTOX®
Licensed in the UK with over 30 years of global experience from across multiple indications1-4
Over 4 years of continued BOTOX® treatment, durable improvements were seen in NDO symptoms and quality of life8
BOTOX® provides sustained reduction in daily episodes of UI and urgency for up to 6 cycles5
BOTOX® is generally well tolerated in NDO5
Safety and tolerability experience from +30 years of use in a range of conditions2, 3, 5, 9, 10
I-QoL: Incontinence-quality of life; NDO: neurogenic detrusor overactivity; UI: urinary incontinence.
Please refer to the BOTOX® Summary of Product Characteristics for further information on adverse events, contraindications and special warnings and precautions for use. The BOTOX® Summary of Product Characteristics can be found here
By clicking the link above you will leave the AbbVie Pro website and be taken to the eMC PI portal website.
Adverse events should be reported. Reporting forms and information can be found at https://yellowcard.mhra.gov.uk/
Adverse events should also be reported to AbbVie on GBPV@abbvie.com
Date of preparation: June 2025. UK-BUO-250044.











.png)
.png)
.png)
.png)
.png)
.png)
